Table of Contents
- 1 What is breast cancer?
- 2 Types of breast cancer (and why type matters on imaging)
- 3 How a breast MRI works
- 4 How MRI is used to detect breast cancer
- 5 How MRI is used for staging and treatment planning
- 6 How MRI is used to monitor treatment and assess recurrence
- 7 When is a Breast MRI recommended?
- 8 What to expect during a breast MRI
- 9 Benefits and limitations (patient-friendly summary)
- 10 References
Breast cancer is a disease in which cells in the breast grow out of control. Most breast cancers begin in the milk ducts or lobules (milk-producing glands) and can spread outside the breast through lymph vessels and blood vessels. When abnormal cells are confined to the ducts or lobules and have not spread into nearby breast tissue, the condition is considered carcinoma in situ (noninvasive). When cancer cells spread into surrounding breast tissue, it is considered invasive and may spread to nearby lymph nodes or other parts of the body.
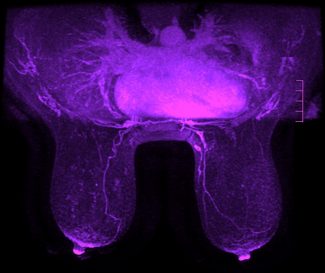
Breast MRI is one of several imaging tools used in breast cancer care. It is not a replacement for mammography or ultrasound; instead, it is typically used as an additional test in specific situations—especially when clinicians need a more detailed map of cancer location, size, and extent.
What is breast cancer?
Breast cancer develops when cells in the breast begin to grow and divide abnormally. Over time, these cells can form a tumor (mass) and, in invasive cancers, can extend into nearby breast tissue. Some breast cancers may also spread to lymph nodes—most commonly in the armpit (axilla)—and to other parts of the body.
Because breast cancer is not a single disease, evaluation usually involves a combination of clinical exam, imaging (mammography, ultrasound, and sometimes MRI), and tissue sampling (biopsy). A biopsy is what confirms the diagnosis and identifies key tumor features that guide treatment.
Types of breast cancer (and why type matters on imaging)
Breast cancers are commonly categorized by where they start and how they grow:
- Ductal carcinoma in situ (DCIS): A noninvasive cancer confined to the ducts. It is often identified on mammography, frequently through calcifications.
- Invasive ductal carcinoma (IDC): The most common invasive type; it begins in the ducts and invades surrounding breast tissue.
- Invasive lobular carcinoma (ILC): Begins in the lobules and can be more subtle on mammography and ultrasound. It may grow in a pattern that makes the true extent of disease harder to estimate with conventional imaging.
Breast cancers are also characterized by biomarkers—such as estrogen receptor (ER), progesterone receptor (PR), and HER2 status. These influence treatment selection (for example, endocrine therapy or HER2-targeted therapy) and contribute to modern staging and prognosis.
How a breast MRI works
A breast MRI uses a powerful magnetic field, radio waves, and a computer to create detailed images of breast tissue—without ionizing radiation. For breast-cancer-related questions, MRI is usually performed with intravenous gadolinium-based contrast. Contrast helps radiologists evaluate tissue enhancement patterns and timing, which can provide additional clues about suspicious findings and the extent of disease.
From a safety standpoint, allergic-like reactions to gadolinium contrast are uncommon, and most reactions, if they occur, are mild. Kidney function may need to be reviewed before contrast is given, particularly in people with known kidney disease. Your imaging center will screen for MRI safety issues, including implanted devices, prior reactions, and relevant medical history.
How MRI is used to detect breast cancer
Breast MRI is valued for its sensitivity and its ability to evaluate the breast in thin “slices,” which can make small or difficult-to-see lesions more conspicuous. Common detection-related uses include:
1) Detecting cancers not clearly seen on mammography or ultrasound
MRI may help identify malignancies that are not visible (or not clearly defined) on standard imaging, including in people with dense breast tissue. Dense tissue can reduce the visibility of abnormalities on mammography, while MRI performance is less dependent on breast density.
2) Further evaluating a finding when standard imaging is inconclusive
In selected cases, MRI is used as a problem-solving tool—particularly when mammography and ultrasound cannot adequately explain a clinical concern or imaging abnormality.
3) Enabling biopsy when the finding is only visible on MRI
If a suspicious area is only visible on MRI, an MRI-guided biopsy may be recommended. This is an important point for patients: imaging can raise or lower suspicion, but biopsy is what confirms cancer.
How MRI is used for staging and treatment planning
“Staging” describes the size of a cancer and how far it has spread. While staging systems are complex, the practical goal is straightforward: staging helps clinicians match the right treatment approach to the true extent of disease.
After a breast cancer diagnosis, a breast MRI may be performed to help clarify:
- Tumor size and local extent
- Whether there are additional tumor sites in the same breast (multifocal or multicentric disease)
- Whether there is unsuspected cancer in the opposite breast
- Whether there are suspicious lymph nodes (especially in the axilla)
These details can influence surgical planning (for example, lumpectomy vs. mastectomy, or the need to localize multiple sites). However, it is important—especially for clinicians—to avoid making definitive treatment changes based solely on MRI appearance when tissue confirmation is feasible. When MRI identifies additional suspicious areas, targeted ultrasound (“second-look” ultrasound) and/or biopsy is often used to confirm the finding before changing the care plan.
How MRI is used to monitor treatment and assess recurrence
Monitoring response to chemotherapy given before surgery (neoadjuvant therapy)
When chemotherapy or other systemic therapy is given before surgery, MRI is often used to evaluate response—how much the tumor has shrunk and whether there is residual disease. This can support surgical planning and help clinicians understand whether treatment is working as intended.
Evaluating the breast after lumpectomy or other prior treatment
Post-treatment changes, such as scarring, can make interpretation on mammography or ultrasound difficult. In appropriate clinical contexts, MRI can help evaluate a concerning change at the surgical site and support decision-making about additional imaging or biopsy.
When is a Breast MRI recommended?
Breast MRI is typically ordered when it can answer a question that mammography and ultrasound cannot, or when it can materially improve treatment planning. Common scenarios include:
- Staging after a new breast cancer diagnosis, especially to define the full extent of disease, evaluate for additional sites in the same breast, or assess the opposite breast.
- Invasive lobular carcinoma (ILC) or other situations where the true extent of disease may be underestimated on mammography or ultrasound.
- Monitoring response to neoadjuvant therapy (treatment given before surgery) to assess residual tumor and guide surgical planning.
- High-risk screening, such as individuals with certain genetic mutations (e.g., BRCA1/BRCA2), a strong family history, or other high-risk factors—often as an annual supplement to mammography.
- Problem-solving when there is a persistent clinical concern or unclear imaging finding and additional detail is needed.
- MRI-only findings that require MRI-guided biopsy because they cannot be targeted on ultrasound or mammography.
Your referring clinician and radiologist will weigh benefits, limitations, and patient-specific factors (including kidney function, device safety, and pregnancy status) to determine whether MRI is appropriate.
What to expect during a breast MRI
Most breast MRI exams take 15 to 60 minutes, depending on the clinical indication and the number of sequences required. You’ll typically lie face down on a padded table designed for breast imaging, and an IV line is placed for contrast administration. The technologist will provide instructions on remaining still and may offer positioning supports to enhance comfort. If you experience claustrophobia, tell your provider in advance. There are practical strategies that can help, ranging from coaching and relaxation techniques to medication when clinically appropriate.
GWIC offers a 1.5T Optima 450W MRI non-claustrophobic scanner with a wider opening that allows entry feet-first and accommodates patients up to 450 pounds.
Benefits and limitations (patient-friendly summary)
Benefits
- Detailed evaluation of tumor size and extent, useful for staging and surgical planning
- Can reveal additional tumor sites in the same breast or an unsuspected cancer in the opposite breast
- Helpful for monitoring the response to therapy given before surgery
- No ionizing radiation
Limitations
- MRI can produce false positives, leading to additional imaging or biopsy that ultimately proves benign
- It is usually supplemental, not a replacement for mammography and ultrasound
- Most breast-cancer applications require contrast, which may not be appropriate in some circumstances (for example, pregnancy)
Contact GWIC for all your MR imaging needs.
References
- National Cancer Institute (NCI). What Is Breast Cancer?
- National Cancer Institute (NCI). Breast Cancer Stages (Staging).
- National Cancer Institute (NCI). Tests for Breast Cancer Biomarkers (ER/PR/HER2).
- RadiologyInfo.org (American College of Radiology & Radiological Society of North America). Breast MRI.
- RadiologyInfo.org (American College of Radiology & Radiological Society of North America). Breast Cancer Screening.
- RadiologyInfo.org (American College of Radiology & Radiological Society of North America). MRI Safety.
- RadiologyInfo.org (American College of Radiology & Radiological Society of North America). MR-Guided Breast Biopsy.
- American College of Radiology (ACR). Practice Parameter for the Performance of Contrast-Enhanced Magnetic Resonance Imaging (MRI) of the Breast.
- American College of Radiology (ACR). Appropriateness Criteria: Monitoring Response to Neoadjuvant Systemic Therapy for Breast Cancer.