Table of Contents
- 1 Coronary Artery Disease and Cardiac MRI
- 2 How MRI helps assess blood flow, ischemia, infarction, and heart muscle damage
- 3 What is coronary artery disease?
- 4 Where cardiac MRI fits in CAD evaluation
- 5 How MRI characterizes an infarction (heart attack) and scar
- 6 Additional ways cardiac MRI can help in CAD-related care
- 7 Who may benefit from cardiac MRI for suspected or known CAD?
- 8 What patients should know before a cardiac MRI
- 9 Important note for patients
- 10 References
Coronary Artery Disease and Cardiac MRI
How MRI helps assess blood flow, ischemia, infarction, and heart muscle damage

Coronary artery disease (CAD) occurs when plaque accumulates in the coronary arteries, reducing blood flow to the heart muscle. Over time, this can lead to chest pain (angina), shortness of breath, decreased exercise capacity, heart attack (myocardial infarction), heart failure, or rhythm disturbances. CAD is also the most common form of heart disease in the United States.
This page expands on the CAD section of Greater Waterbury Imaging Center’s Cardiac MRI service page by explaining how cardiac MRI (also called CMR) is used to assess the effects of CAD on the heart—particularly ischemia (reduced blood flow) and infarction/scar (damage from a previous heart attack)—and to guide treatment decisions. RadiologyInfo states that cardiac MRI is frequently used to evaluate the impacts of CAD, including decreased blood flow and scarring after a heart attack.
What is coronary artery disease?
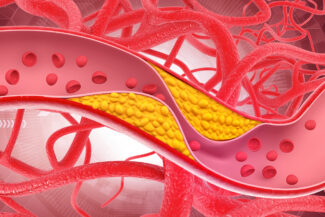
CAD, also known as coronary heart disease or ischemic heart disease, occurs when fatty deposits (plaque) accumulate in the coronary arteries. This process, called atherosclerosis, can restrict or block blood flow to the heart muscle.
Common symptoms may include:
- Chest pain, pressure, or discomfort (angina)
- Shortness of breath
- Fatigue during exertion
- Pain that may radiate to the arm, shoulder, neck, jaw, or upper abdomen
- In some patients, the first apparent sign might be a heart attack.
CAD can be obstructive (significant narrowing of major coronary arteries), nonobstructive, or related to microvascular dysfunction (small vessel disease). NHLBI also notes that coronary microvascular disease is more common in women.
Where cardiac MRI fits in CAD evaluation
Cardiac MRI is a noninvasive imaging test that uses magnetic fields and radio waves (not ionizing radiation) to produce detailed images of the heart. It is especially effective for assessing:
- Heart muscle function and wall motion
- Blood flow to the heart muscle (perfusion)
- Tissue damage, scarring, and viability
- Complications following a heart attack
- Alternative diagnoses when symptoms resemble CAD (in certain cases)
Importantly, MRI is often used to evaluate the effects of CAD on the myocardium (heart muscle) rather than directly visualizing small coronary artery branches. RadiologyInfo notes that detailed coronary artery imaging is generally more challenging with MRI compared to cardiac CT or invasive angiography.
This distinction is clinically significant: CT/coronary angiography can reveal arterial narrowing, while cardiac MRI demonstrates the impact of that narrowing on the heart muscle (e.g., ischemia, scarring, viability, and function). This complementary role is a key reason CMR is valuable for CAD assessment.
How MRI characterizes an infarction (heart attack) and scar
1) Late gadolinium enhancement (LGE): detecting myocardial scar
After gadolinium contrast is administered, cardiac MRI can identify damaged or scarred myocardium using late gadolinium enhancement (LGE) imaging. LGE is a key feature of CMR because it helps distinguish viable myocardium (heart muscle that may recover) from nonviable scar. In ischemic heart disease, the LGE pattern is usually subendocardial (beginning in the inner layer of the heart wall) and follows a coronary artery territory. More extensive or transmural enhancement indicates more severe infarction and less viable tissue.
2) Viability and “recoverability” before revascularization
A classic NEJM study (Kim et al.) showed that the chance of improvement in dysfunctional myocardial segments after revascularization decreases as the transmural extent of hyperenhancement increases. Segments without hyperenhancement were much more likely to improve than segments with extensive (>75%) hyperenhancement. For patients and clinicians, this is highly practical: CMR can help answer not only “Is there damage?” but also “How much of this heart muscle might recover if blood flow is restored?”
3) Risk stratification and prognosis
LGE burden (extent of scarring) and ischemic burden on stress CMR offer valuable prognostic information. Current evidence supports using CMR findings to estimate future cardiovascular risk and guide management decisions.
Cardiac MRI can also assist selected patients by:
- Assessing complications following myocardial infarction (such as adverse remodeling)
- Detecting microvascular obstruction (“no-reflow” zones) within infarcted tissue on LGE imaging, which is linked to poorer prognosis
- Differentiating ischemic scar patterns from non-ischemic patterns when considering other diagnoses (e.g., myocarditis or cardiomyopathy)
Who may benefit from cardiac MRI for suspected or known CAD?
Depending on symptoms, prior testing, and clinical risk, CMR may be considered for patients with:
- Stable chest pain or exertional symptoms
- Known CAD with persistent symptoms despite treatment
- Prior heart attack, where scar/viability assessment is needed
- New or worsening heart failure when ischemic injury is a concern
- Inconclusive prior tests (in certain clinical pathways)
The 2021 AHA/ACC chest pain guideline framework, as summarized in the SCMR perspective, highlights important roles for stress CMR in evaluating intermediate-risk chest pain and in stable chest pain pathways.
What patients should know before a cardiac MRI
Cardiac MRI is noninvasive and does not involve ionizing radiation. Some exams use gadolinium contrast. Patients should inform the imaging team about:
- Pacemakers/defibrillators or other implants
- Kidney disease (important for contrast safety decisions)
- Pregnancy
- Claustrophobia/anxiety
- Prior contrast reactions
RadiologyInfo also notes that image quality depends on remaining still and following breathing instructions, and that some patients may not be candidates for MRI due to device compatibility or other factors.
Important note for patients
If you experience new, severe, or worsening chest pain, shortness of breath, fainting, or symptoms that suggest a heart attack, seek emergency care right away. Cardiac MRI is a valuable diagnostic tool, but emergency assessment—such as an ECG and a troponin blood test—is often the initial step.
GWIC offers MR imaging services in a comfortable setting for fast, accurate results. We have earned the trust of our community and the confidence of physicians to deliver exceptional MR imaging services, including Cardiac MRI and MRI for coronary artery disease.
References
- NHLBI (NIH) – Coronary Heart Disease (What it is / overview), https://www.nhlbi.nih.gov/health/coronary-heart-disease
- CDC – About Coronary Artery Disease (CAD), https://www.cdc.gov/heart-disease/about/coronary-artery-disease.html
- RadiologyInfo.org (ACR/RSNA) – Cardiac MRI (uses, preparation, risks, limitations), https://www.radiologyinfo.org/en/info/cardiacmr
- JAMA Cardiology (2023) – Systematic review/meta-analysis on diagnostic and prognostic value of stress CMR in CAD/stable chest pain, https://jamanetwork.com/journals/jamacardiology/fullarticle/2805949
- SCMR Perspective (PMC, 2022) – Role of CMR within 2021 AHA/ACC Chest Pain Guideline pathways, https://scmr.org/publications/chestpain-guideline/
- Kim et al., NEJM / PubMed (2000) – Contrast-enhanced MRI and myocardial viability/recoverability after revascularization, https://www.nejm.org/doi/full/10.1056/NEJM200011163432003
- PMC review (2024) – LGE patterns, ischemic scar characterization, viability/transmurality, prognostic implications, https://pmc.ncbi.nlm.nih.gov/articles/PMC3946458/
- ESC (2024) – Chronic coronary syndromes guideline overview page (diagnosis and management context), https://www.escardio.org/guidelines/clinical-practice-guidelines/all-esc-practice-guidelines/chronic-coronary-syndromes/